Overview of management of tobacco smoking and nicotine dependence
The guiding principles of managing tobacco smoking are ask, advise, help, as outlined by the Royal Australian College of General Practitioners (RACGP) publication Supporting smoking cessation: A guide for health professionals. This approach is summarised in Approach to screening, assessment and interventions for tobacco smoking.
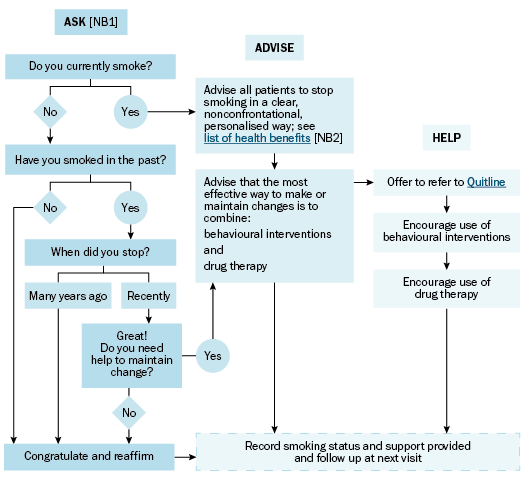
NB1: For more detail, see Screening and assessment of tobacco smoking and nicotine dependence.
NB2: Although the goal of intervention is stopping smoking, for some people, an interim target of cutting down is more achievable, can offer benefit (eg saving money) and can act as a step towards stopping.
Adapted with permission from: Quit. Helping patients to stop smoking: a guide for general practitioners [factsheet]. Version 3.0 (November 2022). https://www.quitcentre.org.au/clinical-tools. Source © 2022 Cancer Council Victoria.
Overview of substance use and addictive behaviours explains key principles of care for a person with a disorder of substance use. Establishing a therapeutic relationship that engages the person (and ideally those close to them) is central to the management of substance use.
Specialist advice on any aspects of care for patients with any disorder of substance use is available and contact is encouraged; see Contact details for substance use clinical advisory services for clinicians.
No amount of tobacco use is considered safe, but making changes to smoking is an achievable step towards stopping. Many people feel demoralised by previous unsuccessful efforts to quit but may be engaged by offers of help to change or control their smoking. Offer patients active assistance and encouragement, whether they are aiming to reduce or stop their smoking or use of nicotine or tobacco. Acknowledging the small wins along the way (the cigarettes not smoked and the money saved) maintains motivation.
Although most literature on managing tobacco use is derived from studies of people who smoke, it is reasonable to apply this to those who use tobacco in other ways because the shared factor perpetuating use is nicotine dependence.
The most effective approach for managing smoking and nicotine dependence is the combination of behavioural interventions and drug therapy. Anyone who uses tobacco or nicotine can benefit from interventions, but highly dependent people are most likely to need drug interventions to make lasting change.
Advise the patient that it is not necessary to set a quit date, although some people prefer to do so. Each patient can decide their rate of reduction, depending on how well their urges to smoke are controlled by the interventions, and their preferences and circumstances.
For patients who have completed the initial course of drug therapy, offer a further course if they wish to continue the drug, as this increases the likelihood of reducing or stopping use and may prevent relapseThe Royal Australian College of General Practitioners (RACGP), 2021. Alternatively, offer a different strategy to promote further attempts at reducing or stopping.
Tobacco smoking affects the metabolism of caffeine1 and many drugs, including antipsychotics (which are most affected), antidepressants, and some antithrombotic drugs (eg warfarin). These pharmacokinetic changes are caused by chemicals in tobacco other than nicotine. Pharmacodynamic drug interactions (interactions that affect the mechanism of a drug’s action) (eg with benzodiazepines) are mainly caused by nicotineLucas, 2013. When a person is reducing or stopping smoking, some medications may require dose adjustment (generally a reduction); for management advice, see Quit Centre’s Clinical tools and guidelines.
Specific considerations are relevant for the management of smoking in people who are pregnant or breastfeeding. For other specific groups, see Considerations for specific populations in substance use and addictive behaviour.
