Starting drug therapy for HFrEF
The suggested approach to management of HFrEF is summarised in Approach to management of HFrEF.
The classes of drugs that improve outcomes in patients with heart failure with reduced ejection fraction (HFrEF) are:
- renin-angiotensin system inhibitors
- heart failure–specific beta blockers
- mineralocorticoid receptor antagonists
- sodium-glucose co-transporter 2 (SGLT2) inhibitors.
Unless contraindicated or not tolerated, start all 4 classes of drugs at diagnosis or within 2 to 4 weeks of diagnosis of heart failure. Good quality clinical evidence shows that these drugs improve survival and reduce hospitalisation for heart failure, and these benefits are seen early (within 30 days of starting treatment). Combination drug therapy improves prognosis and controls symptoms and signs of HFrEF.
For patients with clinical signs of congestion (eg breathlessness, peripheral oedema), defer starting the beta blocker until the patient is euvolaemic.
Increase the doses of the renin-angiotensin system inhibitor and beta blocker every 2 to 4 weeks up to the target or maximum tolerated dose within the recommended range; preferably start all 4 classes of drugs before starting uptitration. The mineralocorticoid receptor antagonist can be uptitrated 4 to 8 weeks after starting, if required.
Optimisation of therapy and achieving target doses may take 2 to 3 months. During this period, assess symptoms, fluid status, kidney function and electrolyte concentrations regularly. Combination drug therapy should be continued even if left ventricular function improves, because there is an increased risk of relapse if therapy is stopped following recovery of left ventricular functionHalliday, 2019.
Patients with persistent symptomatic heart failure, or those unable to tolerate a renin-angiotensin system inhibitor, may benefit from other drug therapies for HFrEF.
Most symptoms and signs of heart failure are due to retention of salt and water and the consequent rise in cardiac filling pressure. Loop diuretics can be added to therapy at any stage to control symptoms of congestion and acute exacerbations. Regularly review the ongoing need for loop diuretics.
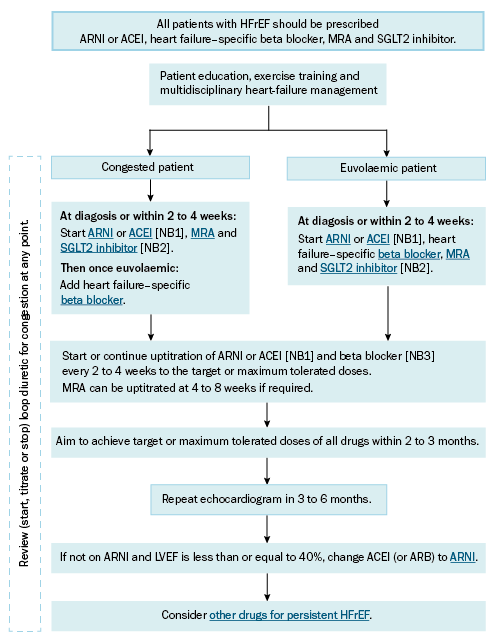
ACEI = angiotensin converting enzyme inhibitor; ARB = angiotensin II receptor blocker; ARNI = angiotensin-receptor neprilysin inhibitor (sacubitril+valsartan); HFrEF = heart failure with reduced ejection fraction; LVEF = left ventricular ejection fraction; MRA = mineralocorticoid receptor antagonist; SGLT2 = sodium-glucose co-transporter 2
NB1: If an ARNI or ACEI is contraindicated or not tolerated, an ARB can be used.
NB2: At the time of writing, the SGLT2 inhibitors with the strongest evidence from outcome studies in patients with HFrEF are dapagliflozin and empagliflozin.
NB3: If the patient has clinical signs of congestion, defer uptitration of the beta blocker until euvolaemic.
